Reflux and Stomach Acid: what you need to know
Let’s talk about reflux or more specifically Gastro Oesophageal reflux disorder (GORD) as I am seeing it increasingly in clinic. If you ever taste acid in your mouth after you eat or you experience burning in the chest portion of your digestive tract this is what I am referring to as reflux. It is a serious condition. Not only does it disrupt quality of life, it can cause irreversible damage to the lining of the oesophegas. Basically, it can ‘burn’ the digestive tract and lead to ulcers and structural changes in the mucous lining. This is not intended to frighten, it’s merely an invitation to be proactive about treatment. Because I know a lot of people put it down to just a normal part of life. But if things are working well, we shouldn’t be dealing with heartburn after every meal.
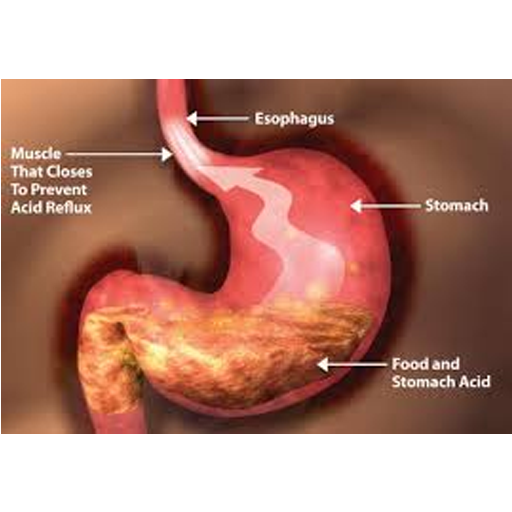
To clarify we have acid that gets produced in our stomachs and allows us to digest all nutrients. Yes the stomach is naturally an acidic environment. Most of the clients I see, seem to have this idea that reflux occurs as a result of excess stomach acid production. Not entirely accurate; GORD is stomach acid in the wrong place i.e. instead of remaining in your tummy its back flowing into your digestive tract. It might be due to over eating, eating foods that don’t agree with you, eating too quickly or lack of tone in the lower sphincter. The sphincter that acts as a barrier between your digestive tract and the entrance to your stomach that is.
Typically, sufferers are recommended proton pump inhibitor therapy (PPI). Think Nexium. These drugs act to block the pathways that stimulate gastric acid secretion (Ament, et. al. 2012) and they are one of the highest selling drugs in Australia and the US so clearly a lot of people are dealing with this issue. While they offer a great deal of relief to sufferers its still important to work out what’s driving the reflux in the first place. Why? Well, stomach acid is kind of important…. consider the following key points:
- Research indicates that stomach acid did in fact evolve to serve as a pathological filter; the pH environment kills microbes (Beasley, et. al. 2015). I.e. stomach acid protects us from bad bugs! This consequence is of most concern in elderly adults already at higher risk of infection.
- It may be more difficult for beneficial microbes to recolonize the gut in a less acidic environment (Beasley, et. al. 2015). Gut health is all the rage right now, hey? And for good reason. Your entire immune system and many of your neurotransmitters are produced there…. so we kind of want to preserve gut health and retain the goodies!
- Prospective trials have shown an increased risk between vitamin B12 deficiency and suboptimal stomach acid. I can attest to this…. most of the clients I see in clinic who have been using PPIs for a long time have shockingly low vitamin B12 levels. B12 plays a critical role in so many functions including mental health, healthy red blood cell production, energy production, cellular renewal and protection against various cancers thus the long term effects of suboptimal B12 may lead to other issues. (N.B. For the biochemistry on this, for those interested consider that pepsin – an enzyme in the belly – is responsible for cleaving B12 from proteins and binding it with R proteins (Heidelbaugh, 2013). I.e. pepsin is needed to make B12 available to the body. And pepsin needs gastric acid to do its job. See the connection?)
- Clinical evidence shows that PPI use reduces the availability of vitamin C in gastric juice and reduces the amount of the active vitamin C available in antioxidant form. Again, vitamin C deficiency has significant consequences to a host of systems in the body (Heidelbaugh, 2013) as its super important.
- Calcium absorption, serum iron levels and magnesium may also be compromised when stomach acid is suboptimal (Heidelbaugh, 2013). Trials seem to suggest that less stomach acid means higher incidence of bone fractures.
This is not an invitation to stop taking a PPI, because you should only do that with your GP’s consent. But it is my little defense case on the importance of stomach acid because as a nutritionist, it kind of all starts there in the gut. And if you don’t have the juice mixed up with your food then you won’t breakdown the nutrients. So… you really aren’t capable of getting much nutritional benefit from your food whatsoever. And given that every hormone, neurotransmitter, enzyme and cell is physically made via the food we eat (this is true on a biochemical level!) then accessing the nutrients your food offers is pretty darn important. Ummm its kind of the key to overall health and keeping everything working in the body. Remember, it all starts with food.
A nutritionist can assist you with doing some preliminary work to ensure that one day you are able to kick the reflux and the drugs as well. Many people that suffer refux have a highly inflammed gastrointestinal tract and may even have ulcers and intestinal permeability which needs to be healed as a priority. Concentrated forms of nutrients including vitamin A, D, slippery elm, the herb liquorice, tumeric and aloe vera are backed by research to support gastrointestinal healing. Don’t do this yourself. Work with a professional. Adding an extra teaspoon of tumeric to your curry won’t do it; you need high quality, high concentration extracted form of the right nutrients in supplement form and these come prescribed by a practitioner. They don’t come from your local supermarket.
There is some neat new research indicating that reflux may be more of an immune mediated reaction then a mechanical one. You can read about that in this article on Medscape here if you are interested. This does not discount the rest of this article, it simply means that down regulating inflammation is important for healing too.
If you are burping up acid and feeling pretty rotten in general then its time to get some help. Drop me an email here or call the clinic on 07 3398 1977 to book.
Note: it is not only PPI’s that change the pH of the stomach. Bariatric surgery involves partial removal of the stomach which may increase the stomach pH to between 5.7 and 6.8. Thus weight loss clients must be supported long term in order to ensure the small amounts of food that they are eating are optimally absorbed. Furthermore, they are at higher risk of microbial overgrowth particularly in the small intestine – SIBO (Beasley, et. al. 2015)
REFERENCES
Cho, C. & Yu, J. (2012). From Inflammation to Cancer. World Scientific, London.
Heidelbaugh, J. (2013). ‘Proton pump inhibitors and risk of vitamin and mineral deficiency: evidence and clinical implications.’ Therapeutic Advances in Drug Safety 4(3). Doi: 10.1177/2042098613482484
Agostan, T,. Dunbar, K., Odze, R. (2016). ‘Association of Acute Gastroesophageal Reflux Disease With Esophageal Histologic Changes’ Journal of American Medicine 315(19).Doi:10.1001/jama.2016.5657
Ament, P. Dicola, D., James, M. (2012). ‘Reducing Adverse Effects of Proton Pump Inhibitors.’ American Family Physician. 86(1). Available from http://www.aafp.org/afp/2012/0701/p66.html