This is a synopsis of the journey of a 50 year old male client of The Balanced Nutritionist who presented with Type 2 Diabetes, hypertension and raised liver enzymes on July 5th 2019. This client wanted to release 25kg of body weight to return to a healthy weight range. In addition, he wanted to minimize his need for medication and better manage his conditions with nutrition and lifestyle. For privacy reasons, this client will be referred to simply as ‘D’ throughout this case study.
The purpose of this report is to draw attention to the power of individualized dietary interventions and professional support in the presence of chronic health conditions. Between the 5th of July and the 12th of October, D released 25kg of body weight, was taken off all diabetes medication (as directed by his GP), significantly lowered his blood pressure medication and improved his overall wellbeing. For the full journey, see below:
Initial consultation July 5th presenting concerns:
- Type 2 Diabetes Mellitus, diagnosed more than 10 years ago. Oral medication (metformin) in use,. Most recent HbA1c* was 11.6
- Blood pressure issues for close to 15 years.
- Triglycerides were 3.2 on latest blood tests despite cholesterol medication.
- Minor reflux
- Occasional muscle cramping particularly in feet
- Uncomfortable with current weight
- Unable to exercise due to shoulder and hip issues
- Energy not ideal particularly in the afternoon
- Family history of blood pressure issues and diabetes type 2
- Motivated to change nutrition and lifestyle to release weight and improve blood pressure and diabetes management.
Initial consultation July 5th Medications and stats:
- Diabetic medication twice daily / blood pressure managed with 2 separate medications taken twice daily / cholesterol medication
- Weight: 124.9kg / waist measurement 114cm
Initial consultation July 5th nutritional and lifestyle habits:
- D was not a big drinker; a couple of nights per week
- Rarely drank soft drink
- Water intake was around 1L
- Plenty of protein in the diet, but perhaps a little too much mindless snacking as a habit – this was most likely driving up blood sugar and making weight loss challenging.
Initial consultation July 5th Initial recommendations:
- Advised to bring in some low impact exercise
- Reduced size of breakfast and asked D to eliminate snacking altogether, focusing on just 3 quality meals
- Increased hydration
- D began logging BSLs* regularly
- D began keeping a food diary which generally helps with more mindful eating by default
Second consultation 3rd August Medications and stats:
- D had followed recommendations to a tee
- BSLs had initially ranged from 8 to 11mmol/L in early July. By the middle of the month they were more often sitting between 5.5 and 7.5mmol/L (readings taken at various times through the day).
- Diabetic mediation reduced and evening blood pressure medication reduced as directed by GP
- Weight 118kg; a reduction of 6kg.
- Waist circumference 110cm; a reduction of 4cm
Second consultation 3rd August Recommendations:
- D embarked on structured Metabolic Balance® program*
- Foods and quantities matched to D based on extensive blood work, medications, medical conditions and physical statistics.
- GP aware and supportive of this dietary approach
Third consultation 23rd August Medications and stats:
- Under direction of GP, metformin (oral diabetic medication) was stopped after 10 years of being mediated for diabetes.
- Fasting BSLs consistently sitting between 4.8 and 5.
- No issues with hypoglycaemia* although blood pressure dipping low at times hence further changes to blood pressure as per below
- Evening BP medication no longer used (as directed by GP)
- Weight reduced to and waist
- Energy fairly consistent, rarely feeling hungry.
- Hamstring pulled unfortunately so not much chance of introducing structured exercise into lifestyle at this point
Third consultation 23rd August Recommendations:
- Continue with structured food plan, addition of more healthy fats
- Keep consulting with GP and keep recording daily blood pressure to ensure medication adjusted accordingly to ensure no low blood pressure episodes.
Fourth consultation 14th September Medications and Stats:
- Current medications consisting only of ½ dose of morning blood pressure pills plus cholesterol pill.
- Still consistently releasing over 1kg of body weight a week, with minimal loss of lean body mass*
- Had introduced a few meals off the plan and noted a fast response to ‘white carbs’ i.e. white rice – a good lesson to learn moving forward*
Fourth consultation 14th September Recommendations:
- Advised to start trialling some foods outside of original plan and monitor blood sugar response particularly to other low GI carbohydrates
- Avoid ‘white’ cabohydrates and high wheat carbs at all costs due to effect on BSL
- Prescribed multi mineral formula to support nutrient status whilst still releasing weight
Fifth consultation 12th October Medications and stats:
- Current weight is 100kg, and according to VLA, body fat is now ideal for frame size. An overall loss of 25kg.
- Waist measurement down to 97cm*, an overall reduction of 17cm.
- D wanting to discuss remaining BP medication and cholesterol medication with GP
Fifth consultation 12th October Recommendations
- Relaxing some aspects of the program with a view of maintain wellbeing and blood sugar readings. Review again in 6 weeks.
- Bring in some exercise with a view for this to become habitual once received the all clear on injuries.
This synopsis of D’s journey so far has been written based on the CARE case report guidelines to ensure the synopsis is as objective as possible. This summary was prepared in consultation with clinical notes taken during consultations. D has read this report in full and confirms it’s accuracy as well as providing consent for it to be published.
The take home points for the reader of this case study include:
- Comprehensive and individualised nutritional prescriptions are a truly powerful solution to chronic and debilitating health conditions
- Food groups don’t necessarily have to be excluded. Exclusions of any whole foods should be based on an individual’s reaction to them – not on a societal level.
- Professional advice and support is critical particularly where medical conditions and medications are involved. D benefited from the support of Katie King, nutritionist as well as his General Practitioner to monitor his medications closely.
- This is not individualised advice. Consult a professional if you want results like this.
- These results are proportionate to effort. We can guide, support and advice but ultimately D had the right mindset to make changes to his nutrition and he deserves these results.
*The term ‘diabetes reversal’ is used in medical literature and the exact criteria for reversal is still debated. However, according to the World Health Organisation, most agree that a HbA1c under the diabetic threshold of 6.5% without the use of medication does qualify. More here: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6520897/
*HbA1c: a test which gives an average of the previous 2-3 months blood sugar results)
*The specific instructions given to this client have been deliberately excluded from this case study as they suited this particular person. The same interventions applied to someone else may not have the same outcome. For safe and effective results, you should work with a suitably qualified practitioner. Book your consultation here.
*BSLs: blood sugar levels
*Metabolic Balance® program is a German medical program that we have received extensive training in and offer at The Balanced Nutritionist. The exact foods and quantities of foods ideal for a person (based on extensive blood work, medications, medical conditions and physical statistics) are prescribed to a person and a structured program follows. Meals are clean, but balanced. Each meal contains protein and fibre rich vegetables as well as fruits and even starch are generally included in a Metabolic Balance® program.
*Hypoglyaemia: low blood sugar (to the extent that it may lead to disturbing symptoms like dizziness, feeling faint, weak or shaky.)
*Lean body mass: the difference between total body weight and fat mass; ideally you always want to preserve lean body mass as it accounts for muscle mass.
*VLA: a scientifically validated test we use in clinic to accurately monitor changes in body fat, lean body mass, hydration and cellular health.
*White carbs: please note that each diabetic is unique. Some, for example may respond fine to fruit others may find it spikes blood sugar. Part of the journey of any diabetic who wants to manage their condition as best as they can through diet, is discovery which foods are most problematic for them. They should then be avoided at all costs.
*Waist measurement: according to the World Health Organisation and the Australian Heart Foundation (https://www.heartfoundation.org.au/your-heart/know-your-risks/healthy-weight/waist-measurement) , a waist measurement is an important measurement of overall risk of chronic disease, particularly cardiovascular disease. Men should strive for a waist measurement below 94cm and women under 80cm.








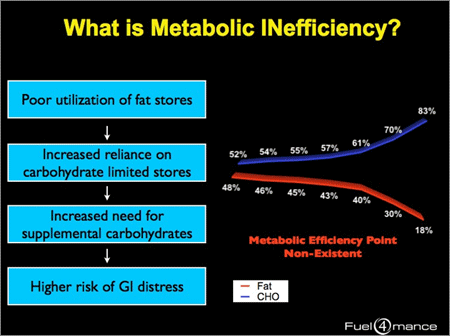 Overall, we know that running a marathon, or doing a triathlon or any type of athletic event is physically stressful – the very process causes a great deal of inflammation within the body. So why then do we turn to copious amounts of highly refined foods that further exacerbate these responses?
Overall, we know that running a marathon, or doing a triathlon or any type of athletic event is physically stressful – the very process causes a great deal of inflammation within the body. So why then do we turn to copious amounts of highly refined foods that further exacerbate these responses?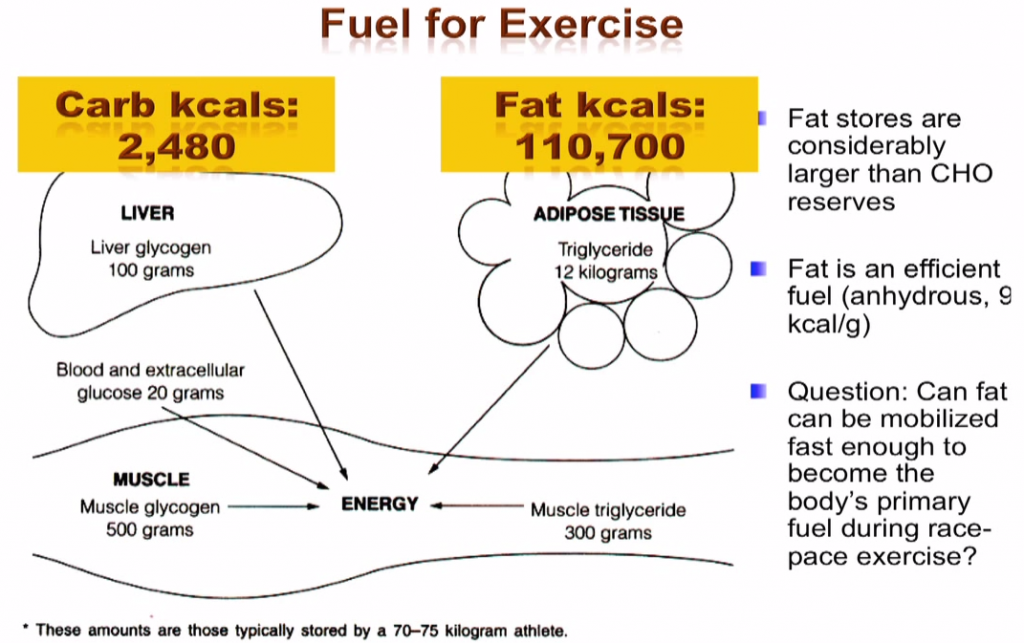 Imagine the potential for athletes who have a continuous fuel source at their disposal? There are lots of athletes out there who are experiencing the benefits; Bevan McKinnon, Sami Inkinen, Bruce Fordyce, Jon Olsen, Zach Bitter and Karyn Hoffman are some of the big names living, breathing and succeeding with this method. But I believe that it is so much more than just performance. I believe that this approach is essential for athletic longevity. It promotes the inclusion of foods in their most unrefined state, with moderate amounts of protein and nourishing anti-inflammatory fats; both of which are essential for hormones, cells and life in general. Interestingly, these ‘real’ food sources are also the richest in nutrients including vitamins, minerals, antioxidants and phytonutrients. As athletes it is absolutely imperative that we are getting an abundance of good nutrition to promote fast recovery, support our immune systems and dampen down inflammation within the body.
Imagine the potential for athletes who have a continuous fuel source at their disposal? There are lots of athletes out there who are experiencing the benefits; Bevan McKinnon, Sami Inkinen, Bruce Fordyce, Jon Olsen, Zach Bitter and Karyn Hoffman are some of the big names living, breathing and succeeding with this method. But I believe that it is so much more than just performance. I believe that this approach is essential for athletic longevity. It promotes the inclusion of foods in their most unrefined state, with moderate amounts of protein and nourishing anti-inflammatory fats; both of which are essential for hormones, cells and life in general. Interestingly, these ‘real’ food sources are also the richest in nutrients including vitamins, minerals, antioxidants and phytonutrients. As athletes it is absolutely imperative that we are getting an abundance of good nutrition to promote fast recovery, support our immune systems and dampen down inflammation within the body.